Imagine telling a patient suffering from age-related (type-II) osteoporosis that a single injection of stem cells could restore their normal bone structure. This week, with a publication in STEM CELLS Translational Medicine, a group of researchers from the University of Toronto and The Ottawa Hospital suggest that this scenario may not be too far away.
Osteoporosis affects over 200 million people worldwide and, unlike post-menopausal (type-I) osteoporosis, both women and men are equally susceptible to developing the age-related form of this chronic disease. With age-related osteoporosis, the inner structure of the bone diminishes, leaving the bone thinner, less dense, and losing its function. The disease is responsible for an estimated 8.9 million fractures per year worldwide. Fractures of the hip — one of the most common breaks for those suffering from type-II osteoporosis — lead to a significant lack of mobility and, for some, can be deadly.
But how can an injection of stem cells reverse the ravages of age in the bones?
Professor William Stanford, senior author of the study, had in previous research demonstrated a causal effect between mice that developed age-related osteoporosis and low or defective mesenchymal stem cells (MSCs) in these animals.
“We reasoned that if defective MSCs are responsible for osteoporosis, transplantation of healthy MSCs should be able to prevent or treat osteoporosis,” said Stanford, who is a Senior Scientist at The Ottawa Hospital and Professor at the University of Ottawa.
To test that theory, the researchers injected osteoporotic mice with MSCs from healthy mice. Stem cells are “progenitor” cells, capable of dividing and changing into all the different cell types in the body. Able to become bone cells, MSCs have a second unique feature, ideal for the development of human therapies: these stem cells can be transplanted from one person to another without the need for matching (needed for blood transfusions, for instance) and without being rejected.
After six months post-injection, a quarter of the life span of these animals, the osteoporotic bone had astonishingly given way to healthy, functional bone.
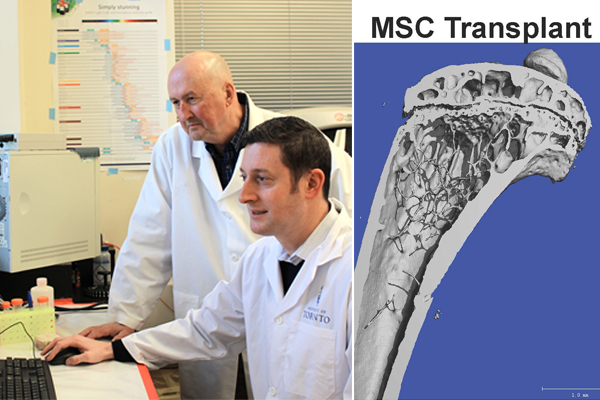
“We had hoped for a general increase in bone health,” said John E. Davies, professor in the Institute of Biomaterials & Biomedical Engineering (IBBME) and the Faculty of Dentistry at the University of Toronto, and a co-author of the study. “But the huge surprise was to find that the exquisite inner “coral-like” architecture of the bone structure of the injected animals—which is severely compromised in osteoporosis—was restored to normal.”
The study could soon give rise to a whole new paradigm for treating or even indefinitely postponing the onset of osteoporosis. Currently there is only one commercially available therapy for type-II osteoporosis, a drug that maintains its effectiveness for just two years
And, while there are no human stem cell trials looking at a systemic treatment for osteoporosis, the long-range results of the study point to the possibility that as little as one dose of stem cells might offer long-term relief.
“It’s very exciting,” said Dr. Jeff Kiernan (IBBME PhD 1T5), first author of the study. Kiernan pursued the research for his doctoral degree, and is now beginning a Postdoctoral Fellowship at The Ottawa Hospital with the Centre for Transfusion Research.
“We’re currently conducting ancillary trials with a research group in the U.S., where elderly patients have been injected with MSCs to study various outcomes. We’ll be able to look at those blood samples for biological markers of bone growth and bone reabsorption,” he added.
If improvements to bone health are observed in these ancillary trials, according to Stanford, larger dedicated trials could follow within the next five years.
Stem cells were first discovered in the early 1960s by University of Toronto Professors James E. Till and Ernest McCulloch. U of T continues to be a world leader in stem cell research, and is home to the world-leading Medicine by Design regenerative medicine research and commercialization program.