Researchers at the University of Toronto (Institute of Biomedical Engineering, Department of Chemistry, Donnelly Centre for Cellular and Biomolecular Research) in collaboration with Sunnybrook Health Sciences Centre, Public Health Ontario, and Mt. Sinai Hospital have engineered a diagnostic test that makes use of a smartphone camera to surveil and track COVID-19 patients.
This finding could significantly improve the turnaround time and efficiency for infectious disease diagnosis, both for COVID-19 and beyond. The research is published in the latest issue of Nano Letters.
“The goal of the study is to make COVID-19 antibody tests more accessible.” said Johnny Zhang, a PhD candidate at the Institute of Biomedical Engineering and Department of Chemistry, and one of the co-first authors of this publication. “The end result is that the patients can take a self-diagnosis for COVID-19 with their phone, and that data can be immediately accessed digitally by medical professionals.”
In a traditional infectious disease diagnostic testing workflow, the clinical sample is obtained from the patient, sent to a laboratory for diagnostic testing, and the result is distributed to clinical personnel for decision making. These processes are often detached in operation and have a long turn-around time.
The researchers engineered quantum dot barcoded microbeads and a secondary label to search for antibodies against COVID-19 antigen in the patient’s blood. Finding the antibodies leads to a change in microbead emission colour.
The beads are then loaded into the device, ‘activated’ with a laser, and the signal is imaged using a smartphone camera. An app is designed to process the image to identify the bead’s emission change. Lastly, the data are interpreted and transmitted remotely across the world for data collection and decision making.
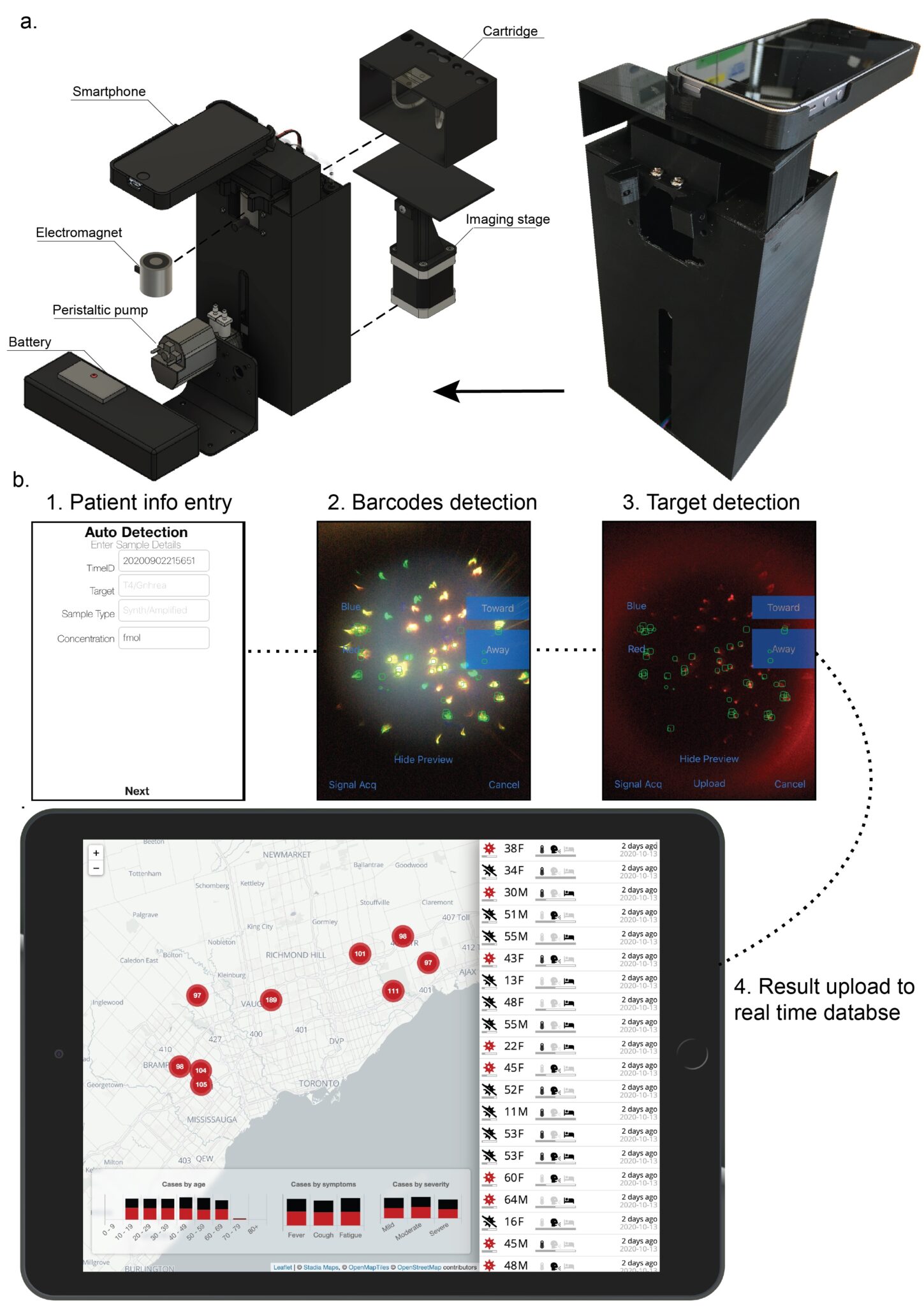
“The beauty of the system is that everything is integrated into one portable unit.” said Zhang.
This technology, by which quantum dot microbead detection can measure minuscule amounts of key biomarkers in blood, has been in development for the past 10 years.
“We really wanted to improve the performance and utility of the technology this time around,” said Ayden Malekjahani (BME PhD candidate), the other co-first author of this study.
“Being able to detect traces of target in patients is not enough. We wanted to add more functions to the device. We designed the device to simultaneously detect multiple antibodies from different sample types, so each test run is packed with information. The results are then uploaded to an online dashboard where medical professionals and the public can see trends in real time.”

The researchers tested this device with forty-nine patient blood samples where varying degrees of COVID-19 infection were present, and were able to achieve 84-88% sensitivity. Although this result is not as high as traditional tests it is still approximately three times higher than lateral flow assays, which are currently the most commonly available portable antibody tests.
This result also means detecting COVID-19 antibody can now be done outside of the centralized facilities without a big drop in accuracy.
This research was a collaboration with the Public Health Ontario, Sunnybrook Hospital and Mount Sinai Hospital, where clinical samples were provided to the researchers to test and evaluate this new system.
“This device can be a game-changer in the way we monitor the spread of infectious diseases and a patient’s response to vaccines.” said Warren Chan, Director and Professor at the Institute of Biomedical Engineering, and the corresponding author of this research.