Whether you fall off your bike and scrape your knee, or knick your finger cutting onions, you know it’s only a matter of time before your injury has scabbed and healed.
But what really just happened – how did your wound actually mend?
Using a student-designed software program called MEDUSA, as well as a special type of microscope and a method called fluorescent tagging, a group of researchers from the Institute of Biomaterials & Biomedical Engineering (IBBME) at U of T have been studying just that.
Published recently in the journal Development, they speculate that they’ve uncovered how some of the fastest wound healers – the embryos of fruit flies – get the job done, in hopes of using their findings to develop medical therapies that aid healing in the future.
Watching wounds mend
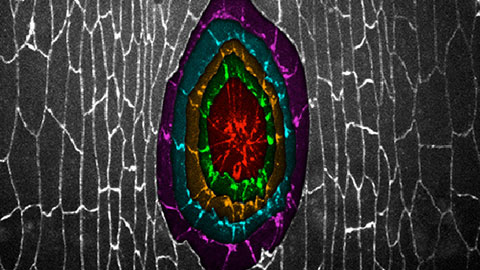
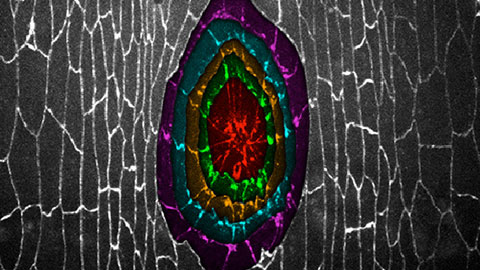
In a typical embryonic wound, a cable-like, cellular structure slowly draws in on itself, eventually closing off the wound in much the same way that a string bag closes. Second-year PhD candidate Teresa Zulueta-Coarasa (PhD IBBME 1T6) examined this behaviour in “normal’ and “mutant” fruit fly embryos.
The goal: to measure how quickly wounds heal over time and what mechanisms lie behind that healing.
It’s an incredibly laborious process. To determine the rate of healing in a single embryo, researchers measure the wound area on each and every frame of a film captured by confocal microscopy. Typically, this involves drawing a polygon shape on the borders of the wound onto hundreds of film images.
To speed the process of discovery, Zulueta-Coarasa developed the MEDUSA software program. The program employs algorithms to automatically find the borders of the wound in a single time frame of film. The resulting contour is then transferred onto the adjacent time frames and fitted to the individual images, making the analysis process for these large amounts of data far more efficient.
The team employed fluorescently-tagged proteins in order to sleuth out the mechanisms behind healing. Molecules that tended to gather around the wound edges increased in intensity, allowing the researchers to

identify specific molecules involved in the healing process.
“We found that for certain proteins, the intensity of the molecule in the wound margin increased rapidly, [suggesting that] those molecules are important to the wound healing process,” said Zulueta-Coarasa.
Helping with healing – from diabetes to cancer
The findings may one day play an important role for those suffering from diabetes or other circulation-related illnesses.
“Patients with chronic wounds heal really slowly or not at all,” explained Zulueta-Coarasa, “but if we could understand why wounds heal so fast in these [fly] embryos, we could develop a strategy to heal them.”
But what surprised the researchers most is that the study may have uncovered a parallel between wound healing and the metastasis of certain cancers.
One of the proteins the researchers saw double in intensity around the wound is called Abelson kinase, or Abl. According to Zulueta-Coarasa, “We have been able to discover that, in mutant embryos without that molecule, wounds still heal – but at a much slower rate.”
Abl, however, is a molecule more commonly associated with metastatic cancers.
“From a biomedical perspective,” explained Assistant Professor Rodrigo Fernandez-Gonzalez (IBBME), corresponding author on the paper, “the identification of a role for the protein Abl in coordinated cell migration [during wound healing] generates new hypotheses about its role in metastasis.”
“Abl activation is associated with invasive breast cancer, in which small groups of cells can coordinate their migratory behaviours to spread disease,” he added.
Though intriguing, the connection between the molecule’s role in speeding up the healing process and spreading cancer remains a mystery. “The actual mechanisms by which Abl promotes metastasis are unclear,” said Fernandez-Gonzalez.
For now, the team hopes to better understand the science behind the healing process, one tiny nick at a time.